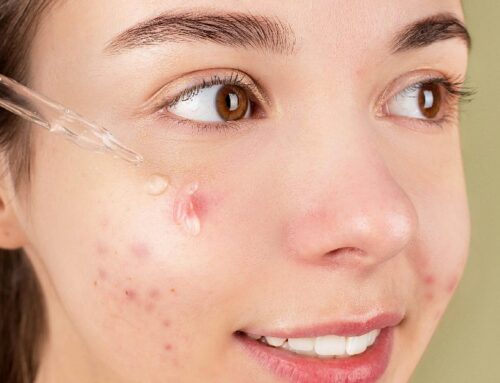
Most of us were promised that acne would end with adolescence. For a significant number of people — particularly women — that promise was never kept. Adult acne (defined as acne persisting or appearing after age 25) affects up to 50% of women in their 20s and 25% in their 40s. It’s increasingly common, increasingly poorly managed, and carries a disproportionate psychological burden because there’s a persistent and unfair narrative that ‘adults shouldn’t have acne.’
Here’s what’s actually happening — and what we can do about it.
Why Adults Get Acne (And Why It’s Different From Teenage Acne)
Teenage acne is largely driven by puberty — a surge in androgens causes sebaceous glands to overproduce sebum, which clogs follicles, creates the conditions for Cutibacterium acnes (the acne-causing bacterium) to thrive, and triggers inflammation.
Adult acne, particularly in women, has a more complex hormonal landscape:
Hormonal fluctuations: The classic presentation is cyclical breakouts that worsen in the week before menstruation. This is driven by progesterone peaks and relative oestrogen declines, which stimulate sebum production. Women with PCOS (polycystic ovary syndrome) frequently present with acne as a primary complaint, often accompanied by irregular periods and excess facial hair.
High cortisol (stress): The adrenal glands produce androgens in response to stress. Sustained high-stress environments — something many Indian professionals in their 20s and 30s live with chronically — directly stimulate sebum production and impair the skin’s barrier function.
Comedogenic skincare and makeup: Many adults develop acne from the very products they’re using to address their skin concerns. Silicones, certain mineral oils, and occlusive agents in moisturisers and foundations are common culprits.
Dietary factors: The evidence for dairy (particularly skim milk) and high-glycaemic foods triggering acne has strengthened considerably over the past decade. This is particularly relevant in the Indian context, where refined carbohydrates and dairy are dietary staples.
Why OTC Products and Home Remedies Fail
Walk into any pharmacy and you’ll find shelves of benzoyl peroxide washes, salicylic acid face washes, and niacinamide serums marketed for acne. These can help mild comedonal acne, but they are insufficient for moderate to severe inflammatory acne for several reasons:
OTC concentrations are limited. Prescription benzoyl peroxide formulations are significantly more effective than cosmetic ones. Treating the surface doesn’t address the root. If your acne is driven by hormonal imbalance, the best benzoyl peroxide wash in the world won’t stop new breakouts — it can only manage what’s already surfaced. Unsystematic treatment creates antibiotic resistance. Many adults self-treat with OTC antibiotic creams intermittently, which contributes to C. acnes resistance and makes future treatment harder. Home remedies including lemon juice, toothpaste, baking soda, and raw honey can disrupt your skin’s microbiome and pH and worsen the very condition they’re meant to treat.
The Dermatologist’s Approach to Adult Acne
When a patient presents with adult acne at our clinic, our approach is:
- Classify the acne: Is it predominantly comedonal (blocked pores), papular/pustular (inflammatory), nodular/cystic (deep, painful), or post-inflammatory (PIH and scarring)? Each responds to different treatments.
- Identify the drivers: Hormonal history, menstrual cycle correlation, stress levels, current skincare and makeup, diet, and family history are all assessed.
- Build a tiered treatment plan:
For mild-moderate acne: A prescription topical regimen typically combining retinoids (adapalene or tretinoin) with an antibiotic (clindamycin) or benzoyl peroxide. Retinoids are the single most evidence-backed topical treatment for acne — they normalise follicular keratinisation, reduce sebum, and improve post-acne pigmentation.
For moderate-severe acne: Oral antibiotics for limited courses (doxycycline is most commonly used in India) combined with topicals. We are careful to limit antibiotic duration to reduce resistance.
For hormonal acne in women: Oral contraceptives or spironolactone can be dramatically effective for cyclical, hormonal breakouts. These are systemic treatments that work at the root cause rather than the surface.
For severe nodular/cystic acne: Isotretinoin (Accutane) remains the only treatment capable of achieving long-term remission of severe acne. It carries side effects that require monitoring, but for the right patient, it’s genuinely life-changing.
- Address active acne and scarring simultaneously: We frequently combine acne treatment with early intervention for scars — chemical peels and microneedling can begin once active acne is controlled, reducing long-term scarring burden.
A Word on Prescription Medications from Instagram
There is a growing trend of people self-prescribing tretinoin, spironolactone, or even isotretinoin based on social media recommendations. Please don’t. These are powerful medications with real side effects and contraindications. Tretinoin can cause severe purging if introduced incorrectly. Isotretinoin is teratogenic (harmful to foetal development) and must be used with stringent contraception protocols in women of childbearing age. Spironolactone requires blood pressure and potassium monitoring. A dermatologist doesn’t just prescribe these — we monitor you through the process.
You Don’t Have to Live With This
Adult acne is not a character flaw or a result of poor hygiene. It’s a medical condition with identifiable causes and proven treatments. The vast majority of patients who come to our clinic with chronic adult acne see significant improvement within 3–4 months of a structured treatment plan.
If you’ve been managing your acne with home remedies and OTC products for years, it’s time to try something that actually works.
Book a consultation at Dr. Nishita’s Clinic: wa.me/919381218003