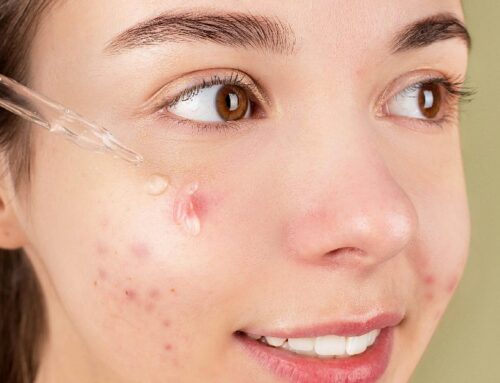
If your skin is simultaneously oily and dehydrated, breaking out and flaking, or burning when you apply products that never used to sting — your skin barrier is likely compromised. This is one of the most common presentations we see at our clinic, and it is almost always either caused or worsened by the patient’s own skincare routine.
The skin barrier is not a marketing term. It is a clinically defined structure, and when it fails, the consequences go well beyond dryness. Here is what is actually happening — and what it takes to repair it.
What the Skin Barrier Actually Is
The outermost layer of your skin — the stratum corneum — functions as a physical and chemical barrier between your body and the environment. Structurally, it is often described as a brick-and-mortar system: corneocytes (dead skin cells) are the bricks, and a lipid matrix composed primarily of ceramides, cholesterol, and fatty acids is the mortar.
This barrier does two critical jobs: it keeps water inside the skin (preventing transepidermal water loss, or TEWL) and it keeps irritants, allergens, bacteria, and pollutants out. When the lipid matrix is disrupted — through over-exfoliation, harsh surfactants, incorrect actives, environmental stress, or illness — both functions fail simultaneously.
The result: dehydration, sensitivity, inflammation, and in many cases, secondary infections or acne, because a compromised barrier is an open door for Cutibacterium acnes and other pathogens.
How Barriers Get Damaged — and Why Indian Skin Is Particularly Vulnerable
The single most common cause of barrier damage we see in our clinic is over-exfoliation. The skincare content ecosystem — Instagram, YouTube, dermatology influencers — has created a culture of aggressive exfoliation that is fundamentally incompatible with Indian skin types.
Fitzpatrick III–V skin, which accounts for the majority of the Indian population, has a higher inflammatory response to barrier disruption than lighter skin types. This means that the same AHA concentration, the same physical scrub, the same retinol dose that a person with lighter skin tolerates without incident can trigger significant inflammation, post-inflammatory hyperpigmentation, and prolonged barrier dysfunction in Indian skin.
Other common causes: switching products too frequently, layering multiple actives without understanding interactions, using foaming cleansers with high pH (most Indian drugstore cleansers sit at pH 8–10 when the skin’s natural pH is 4.5–5.5), and extended use of steroid-based creams — a significant problem in India given the availability of potent topical steroids over the counter.
How to Know Your Barrier Is Damaged
The signs are often mistaken for other conditions, which leads to incorrect treatment and further damage. Barrier dysfunction typically presents as one or more of the following: a tight, uncomfortable sensation after cleansing; stinging or burning when applying serums or moisturisers that previously caused no reaction; simultaneous oiliness and flakiness (the skin is producing excess sebum to compensate for lost lipids while the surface remains dry); redness or persistent low-grade irritation with no clear cause; and sudden sensitivity to products used for months without issue.
At our clinic, we assess barrier health as part of every consultation — because treating pigmentation, acne, or ageing on a compromised barrier is counterproductive. The barrier must be restored before any active treatment can work effectively.
What Actually Repairs a Damaged Skin Barrier
The repair protocol is unglamorous, and patients often resist it because it requires stopping most of what they are currently doing. But it works.
The first step is stripping the routine back to three products: a gentle, low-pH cleanser (ideally pH 5–5.5), a ceramide-rich moisturiser, and sunscreen. Nothing else. No actives, no exfoliants, no vitamin C, no retinol. The barrier cannot repair itself if it is under constant chemical stress.
Ceramide-containing moisturisers are the clinical standard for barrier repair. Ceramides are the dominant lipid in the stratum corneum, and topical application has been demonstrated to accelerate barrier recovery. Look for formulations that combine ceramides with cholesterol and fatty acids in a ratio that mimics the natural skin lipid profile — this combination outperforms ceramides alone.
Hyaluronic acid is useful for hydration but does not repair the barrier on its own. It attracts water to the skin’s surface but cannot replace lost lipids. In dry climates or air-conditioned environments, hyaluronic acid without an occlusive layer on top can actually increase TEWL. Always seal it with a lipid-rich moisturiser.
Timeline for repair: a mildly compromised barrier typically shows meaningful improvement in 2–4 weeks with the correct protocol. A significantly damaged barrier — from months of over-exfoliation or steroid misuse — can take 8–12 weeks. Patience is non-negotiable.
When to See a Dermatologist
If your skin has been reactive, sensitive, or persistently inflamed for more than four weeks despite simplifying your routine, it is time to see a dermatologist. What presents as barrier damage can sometimes be rosacea, seborrhoeic dermatitis, perioral dermatitis, or contact allergic dermatitis — conditions that require specific treatment, not just a simplified routine.
We also see a significant number of patients who have self-treated barrier damage with products marketed as “barrier repair” but formulated with fragrances, essential oils, or alcohol — ingredients that actively worsen barrier function. Over-the-counter is not always safe, and in dermatology, more expensive rarely means more effective.
If you are unsure whether what you are experiencing is barrier damage or another condition, a skin consultation is the fastest way to get a clear answer and a protocol that actually works for your skin type.
Book a consultation at Dr. Nishita’s Clinic: +91 93812 18003
— Dr. Nishita Ranka | Consultant Dermatologist | Dr. Nishita’s Clinic for Skin, Hair & Aesthetics, Hyderabad