Pregnancy causes profound hormonal changes that affect every organ — including the skin. Many of these changes resolve spontaneously after delivery and during breastfeeding. Others persist and require treatment. Understanding the difference — and knowing when it is safe to intervene — is something we address regularly in consultations with postpartum patients.
Melasma
Pregnancy-induced melasma — the “mask of pregnancy” — affects up to 70% of pregnant women and is driven by oestrogen and progesterone-mediated upregulation of melanocyte activity. In Indian skin, which already has higher baseline melanocyte activity, pregnancy melasma can be particularly pronounced. The good news: for many women, it fades significantly after delivery and with consistent sun protection. The less good news: in a significant proportion of patients, particularly those with a strong genetic predisposition or who have not been rigorous with sunscreen during pregnancy, melasma persists and requires active treatment. Treatment — topical agents including azelaic acid, kojic acid, tranexamic acid, and later tretinoin — is safe to commence after breastfeeding ends. In-clinic treatments (chemical peels, lasers) are considered after the breastfeeding period.
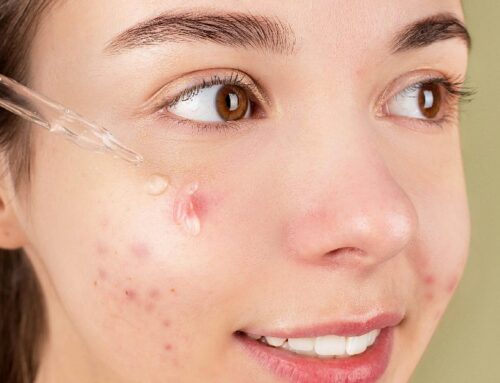
Acne
Postpartum acne is common — driven by the hormonal fluctuations that occur in the months after delivery, particularly the drop in progesterone. For breastfeeding mothers, treatment options are limited: topical azelaic acid and clindamycin are safe; tretinoin, oral isotretinoin, and most oral antibiotics are not recommended while breastfeeding. Patients who are not breastfeeding have broader treatment options available sooner.
Stretch Marks
Striae gravidarum — stretch marks from pregnancy — are easier to treat when they are still in the red/purple phase (striae rubra) than when they have matured to white/silver (striae alba). Early intervention with microneedling, MNRF, or fractional laser produces meaningfully better outcomes. We advise patients to begin treatment discussions 3-6 months postpartum, once the skin has stabilised and breastfeeding status is known.
Hair Loss
Postpartum telogen effluvium — shedding in the 3-6 months after delivery — is extremely common and almost universally temporary. It requires reassurance more than treatment in most cases, though iron and vitamin supplementation are important given the nutritional demands of pregnancy and breastfeeding. Persistent or severe hair loss beyond 12 months postpartum warrants investigation for thyroid dysfunction, iron deficiency anaemia, or the development of androgenetic alopecia.
Book a consultation: wa.me/919381218003
— Dr. Nishita Ranka | Consultant Dermatologist | Dr. Nishita’s Clinic for Skin, Hair & Aesthetics, Hyderabad