By Dr. Nishita Ranka Bagmar, MBBS DDVL | Medical Director, Dr. Nishita’s Clinic For Skin, Hair & Aesthetics, Hyderabad
Here’s a number that should stop you mid-scroll: in a 2022 survey by the Indian Journal of Dermatology, hyperpigmentation was the single most common reason Indian adults sought a dermatologist — ahead of acne, hair fall, and rashes combined. Nearly 1 in 3 women in India reports pigmentation as their primary skin concern.
And yet, most of them are spending money on the wrong things. Creams that quietly damage the skin barrier. DIY hacks that trigger more inflammation. Parlour bleach sessions that make the problem worse over summer. “Fairness” treatments that are neither fair nor treatments.
As a dermatologist who sees pigmentation every single day — in patients from their teens to their eighties, across all Indian skin types — I want to give you the honest clinical breakdown. What pigmentation actually is. What causes it. And most importantly: what genuinely works, what doesn’t, and why April in Hyderabad is exactly the wrong time to start certain treatments without the right protection.
What Is Pigmentation, and Why Are Indian Skin Types More Vulnerable?
Pigmentation is any change in skin colour caused by an excess (or absence) of melanin — the pigment produced by melanocytes, specialised cells in the deepest layer of your skin.
Indian skin falls predominantly in Fitzpatrick Types III, IV, and V — meaning our skin has significantly more melanocytes, and those melanocytes are hyperreactive. This is evolutionary: more melanin = more protection against the fierce South Asian sun. But it comes with a tradeoff. Our skin responds to any insult — a pimple, a scratch, friction from a tight dupatta strap, or a sunburn — by producing excess melanin at the site of injury.
In lighter Fitzpatrick skin types (I-II), the same injury might fade within weeks. In Indian skin, it can linger for months, sometimes years, without targeted treatment.
This is not a flaw. It’s biology. But it means that treating pigmentation on Indian skin requires a completely different protocol than what Western skincare brands are designed for — and most of what you read online is written for Fitzpatrick I-III.
The Main Types of Pigmentation on Indian Skin
Not all dark spots are the same. Getting the diagnosis right is the first step to getting the treatment right. Here’s what I see most frequently in clinic:
1. Melasma
The most stubborn of them all. Melasma presents as symmetric, brown-grey patches — typically on the cheeks, upper lip, forehead, and chin. It’s driven by a combination of UV exposure, hormonal fluctuations (oestrogen and progesterone), and genetic predisposition.
Melasma is especially common in: – Women during pregnancy (“mask of pregnancy”) – Women on oral contraceptive pills – Anyone with significant daily sun exposure without adequate protection
The cruel irony of melasma: it worsens dramatically in summer, and aggressive treatments (like high-strength peels or laser) without proper sun protection can trigger a rebound flare worse than the original. More on this shortly.
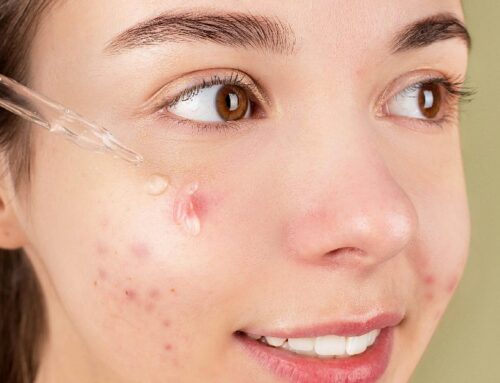
2. Post-Inflammatory Hyperpigmentation (PIH)
This is the dark mark left behind after acne, a cut, an allergic reaction, or even a waxing rash. PIH is extremely common in Indian skin because of our hyperreactive melanocytes. It’s technically not a “scar” — the skin texture is normal — but the discolouration can be deep and persistent.
Read more about acne-related pigmentation here →
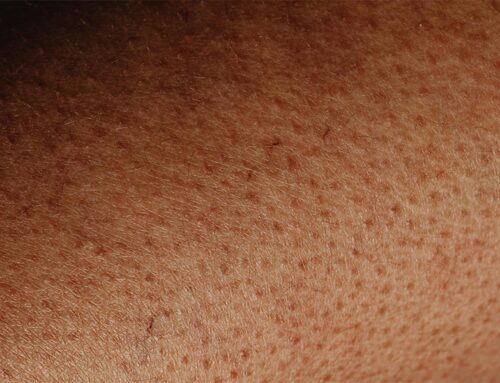
3. Solar Lentigines (Sun Spots / Age Spots)
Discrete, flat, brown spots that appear on sun-exposed areas — face, neck, forearms, hands. They’re caused by cumulative UV damage over years. In Hyderabad, where UV index regularly hits 10-11 in summer, these can appear as early as your late twenties without daily SPF 50+ PA++++.
More on uneven tone and sun tanning →
4. Periorbital Pigmentation (Under-Eye Circles)
Dark circles in Indian skin are largely constitutional — meaning genetic. Brown-toned under-eye pigmentation is different from the bluish-purple circles caused by thin skin or poor circulation. Understanding which type you have determines which treatment will actually help.
More on pigmentation patterns →
5. Freckles and Ephelides
Smaller, discrete spots triggered by sun exposure. More common in lighter-skinned Indians. Unlike lentigines, these fade significantly in winter and with consistent sun protection.
What Triggers Pigmentation — and Makes It Worse
Understanding your triggers is half the battle:
- UV exposure: The #1 driver of all forms of pigmentation. Hyderabad’s summer UV index means even 15 minutes of midday sun without SPF 50+ PA++++ can undo weeks of treatment.
- Hormonal changes: Pregnancy, postpartum period, hormonal contraceptives — all increase melasma risk significantly.
- Post-inflammatory triggers: Acne, ingrown hairs, waxing, rough facial scrubs, popping pimples. Every inflammatory episode is a potential dark mark.
- Heat: Infrared radiation from heat (stoves, direct sun, saunas) can independently stimulate melanin production — separate from UV. This is why some melasma patients flare even indoors near windows.
- Friction: Rubbing the face, tight clothing on the neck, certain accessories. Repeated friction = repeated inflammation = repeated pigmentation.
- Certain medications: Some antibiotics, antiepileptics, and NSAIDs can cause drug-induced pigmentation.
What Doesn’t Work (Please Stop Spending Money on These)
This section might sting a little. But I’d rather tell you the truth.
Skin-Lightening Creams with Harmful Ingredients
India’s over-the-counter market is flooded with creams containing high-dose steroids, mercury, and undisclosed hydroquinone — all sold legally or semi-legally under various brand names. These can initially “lighten” skin by suppressing inflammation, but long-term use causes: – Steroid-induced skin thinning (atrophy) – Perioral dermatitis – Paradoxical darkening on withdrawal – Mercury toxicity with systemic use
The CDSCO has issued warnings, but enforcement is inconsistent. If a cream promises visible results in 7 days, read the ingredient list very carefully.
Turmeric, Lemon Juice, and Kitchen DIY Hacks
I have nothing against kitchen ingredients in general. But applying raw lemon juice to your face in Hyderabad summer is genuinely dangerous — it’s phototoxic, meaning it sensitises skin to UV and can cause severe, uneven burns and pigmentation on UV exposure. Turmeric can stain and is poorly studied for clinical hyperpigmentation.
Parlour Bleach and Chemical Facial Treatments
Bleach contains hydrogen peroxide, which temporarily oxidises melanin (making it appear lighter) without addressing the underlying cause. The results last days. The irritation can last much longer — and repeated bleach sessions are a common PIH trigger in Indian skin.
Single-Ingredient “Quick Fix” Serums Without Medical Supervision
Vitamin C serums, kojic acid creams, and niacinamide products can absolutely help — but which one, at what concentration, in which combination, and in what order matters enormously. Randomly layering actives is one of the fastest ways to trigger irritant reactions and more PIH in Indian skin.
What Actually Works: The Evidence-Based Approach
Here’s the honest breakdown of treatments with real evidence behind them:
Topical Actives (First Line)
Niacinamide (Vitamin B3) One of the safest, best-tolerated brightening agents. Inhibits melanosome transfer (the process by which melanin moves into skin cells). Excellent for PIH and early melasma. Works beautifully in Indian skin because it doesn’t cause the irritation that retinoids can.
Azelaic Acid Underrated and underused. Clinically proven for melasma, PIH, and rosacea-associated redness. It inhibits tyrosinase (the enzyme that drives melanin production) selectively — meaning it targets hyperpigmented cells without affecting normal skin tone.
Tranexamic Acid A newer addition to the dermatologist’s toolkit with impressive evidence for melasma — both topically and in oral low-dose form (the latter requires prescription and medical supervision). Inhibits UV-induced prostaglandin synthesis, which is one of the key pathways in melasma.
Kojic Acid Traditional but effective tyrosinase inhibitor. Often combined with other actives in prescription formulations. Can be sensitising at high concentrations — which is why dermatologist-supervised use is recommended.
Vitamin C (L-Ascorbic Acid) + Vitamin E A powerful antioxidant combination that neutralises UV-induced free radical damage and inhibits melanin production. Needs to be formulated correctly (stable pH, appropriate concentration) — which is where many OTC products fall short.
Retinoids Effective for pigmentation by accelerating cell turnover, but must be used with extreme caution in Indian skin during summer. Retinoids increase photosensitivity — meaning sun protection becomes even more non-negotiable. Not ideal to start in April-May without rigorous sun protection discipline.
In-Clinic Treatments
Chemical Peels From superficial (lactic, mandelic) to medium-depth (TCA), peels accelerate the shedding of pigmented skin cells and stimulate fresh cell turnover. The key word is supervised — the wrong peel strength or formulation on Indian skin can cause a PIH flare that’s worse than the original pigmentation.
Mandelic acid peels are particularly well-tolerated in Indian skin (Fitzpatrick III-V) — larger molecule, slower penetration, lower irritation risk.
Q-Switch Nd:YAG Laser The gold standard for superficial pigmentation, lentigines, and certain types of melasma. Works by selectively targeting melanin with specific wavelengths, leaving surrounding tissue unaffected. At our clinic, we use the Bi-Axis Q-Switch system, which allows precise targeting.
Multiple sessions are typically needed. Critically: Q-Switch laser in summer without rigorous SPF 50+ PA++++ maintenance = wasted money and potential PIH. Post-laser sun protection is non-negotiable.
PicoSure / PicoLaser Picosecond lasers deliver energy in ultra-short pulses, shattering pigment particles more efficiently with less heat than traditional Q-Switch. Better for stubborn melasma and dermal pigmentation. Also more expensive — and still requires rigorous sun protection as part of the protocol.
Combination Protocols In my clinical experience, no single treatment gives the best results for Indian skin. The most effective approach combines: – A targeted topical regimen (personalised to your pigmentation type) – In-clinic treatments timed appropriately with seasonal UV intensity – Strict daily sun protection (SPF 50+ PA++++) – Maintenance between sessions
More on skin concerns and anti-ageing →
The Summer Warning: Why April-May Is a Critical Window
I want to be direct: April and May in Hyderabad are among the worst months to start aggressive pigmentation treatment — unless you have a non-negotiable sun protection routine in place.
Here’s why: – UV index peaks at 10-11 in Hyderabad from April through June – Outdoor UV exposure even for 10-15 minutes at midday can counteract weeks of treatment – Aggressive treatments (medium-depth peels, laser, retinoids) make skin more photosensitive — any UV exposure during recovery can trigger PIH – Heat-induced melasma flares independently of UV — so even air-conditioned environments with window light can be a trigger
This does not mean do nothing in summer. It means: – Do start: A gentle, dermatologist-supervised topical regimen (niacinamide, azelaic acid, tranexamic acid) – Do continue: Any ongoing laser programme with strict sun protection – Don’t start: New aggressive peels or first-time laser in peak summer without establishing sun protection habits first – Do obsess about: SPF 50+ PA++++ every single morning, reapplied every 2-3 hours if outdoors
Sunscreen is not optional. It is the most powerful anti-pigmentation tool you have — and the only one that works preventively.
How I Approach Pigmentation at Dr. Nishita’s Clinic: Diagnosis First
I’ll tell you what separates dermatologist-managed pigmentation care from everything else: we diagnose before we treat.
Melasma, PIH, and solar lentigines look similar to an untrained eye but respond to completely different treatments. Treating melasma like PIH can cause a flare. Treating PIH aggressively with the wrong peel can deepen it. And treating constitutional periorbital pigmentation with topicals alone is a waste of time — it needs a combination approach including injectables.
When a patient comes to my clinic for pigmentation, here’s what happens: 1. Detailed history: Hormonal status, sun exposure habits, current skincare, medications 2. Clinical examination: Type, depth, and distribution of pigmentation 3. Wood’s lamp examination if needed: Distinguishes epidermal from dermal pigmentation — which directly determines treatment response 4. Personalised protocol: Topicals + in-clinic + sun protection + timeline, tailored to your skin type, your pigmentation type, and your lifestyle
There is no one-size-fits-all. And there should never be.
The Bottom Line
Pigmentation on Indian skin is real, it’s common, and it’s treatable — but not with shortcuts. The most powerful thing you can do starting today: SPF 50+ PA++++, every morning, no exceptions. It’s the single intervention with the most evidence behind it, the least risk, and the broadest benefit.
Beyond that, the path forward is diagnosis and a personalised protocol — because your melasma is different from your neighbour’s dark spots, and they need different treatment.
Ready to Get Your Pigmentation Properly Diagnosed?
If you’re tired of guessing, wasting money on the wrong products, and watching dark spots that just won’t budge — it’s time for a proper clinical assessment.
Book a consultation at Dr. Nishita’s Clinic For Skin, Hair & Aesthetics, Hyderabad.
Dr. Nishita Ranka Bagmar (MBBS DDVL) is a board-certified dermatologist and international trainer with over a decade of clinical experience treating pigmentation across all Indian skin types.
📍 Hyderabad | 📞 Book via drnishitaranka.com
Don’t treat the symptom. Treat the cause.
References: – Sarkar R et al. Melasma in Indian patients: A clinical, histopathological and Wood’s lamp study. Indian J Dermatol Venereol Leprol. 2020. – Rodrigues M et al. Hyperpigmentation in skin of colour: Mechanisms and management. J Eur Acad Dermatol Venereol. 2022. – AAD Guidelines on Melasma Treatment. 2023. – Sheth VM, Pandya AG. Melasma: a comprehensive update. J Am Acad Dermatol. 2011.